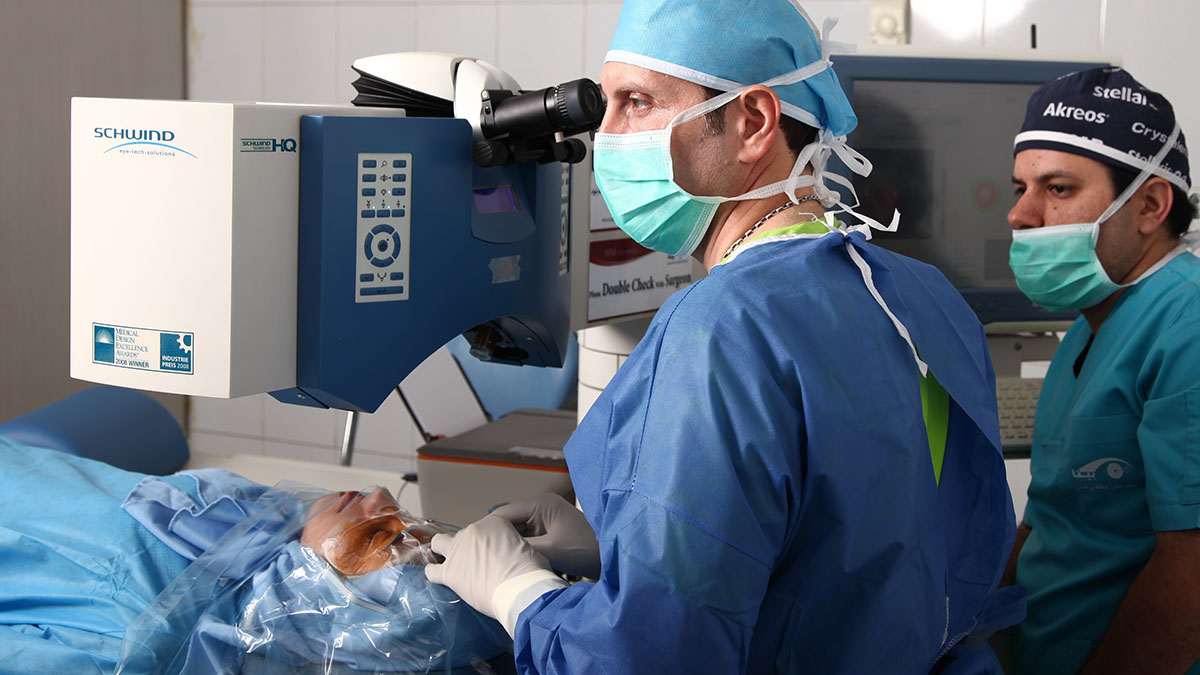
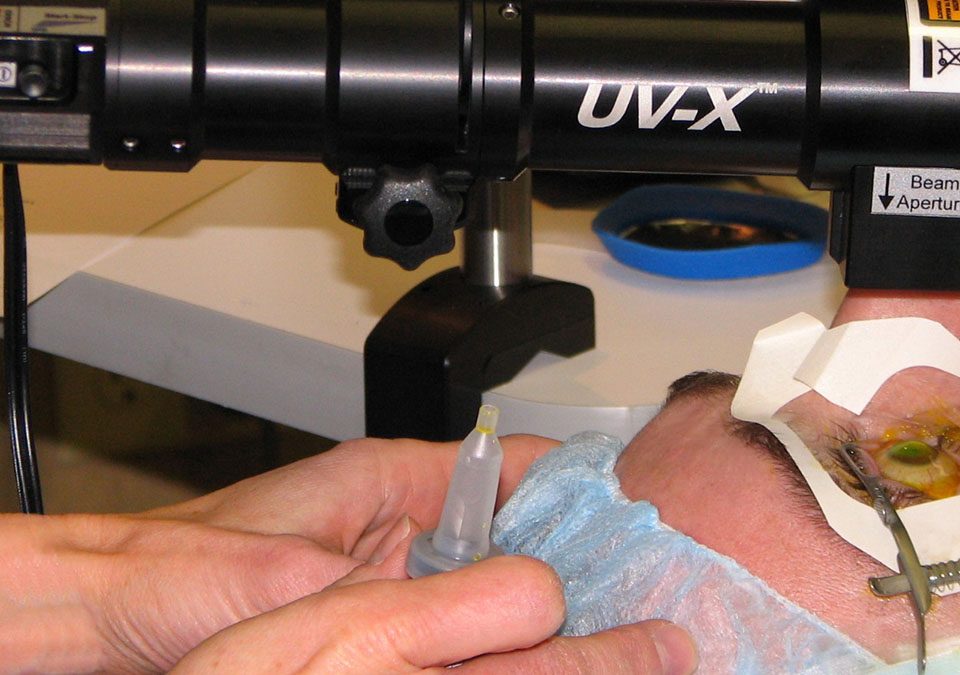
Lasik, Lasek, TransPRK, Femtolasik
Lasik vs. Lasek
LASIK is a laser vision correction procedure that treats refractive errors, such as nearsightedness (myopia), farsightedness (hyperopia), and astigmatism (oval curvature), etc. by removing corneal tissue beneath the surface of the cornea.
During the LASIK procedure, a flap is created on the surface of the cornea. A computer-controlled excimer laser is then used to remove the proper amount of corneal tissue. In less than one minute, the excimer laser reshapes the internal cornea or stroma. The thin flap of corneal tissue is then folded back into its original position, where it bonds after only a few minutes of drying.
On the other hand, no flap is created with LASEK surgery. Instead, the surgeon simply loosens the top layer of the cornea and moves it aside. After the laser has finished, this outer layer (the epithelium) is carefully placed back and left to heal over time.
Femtolasik
FEMTOLASIK is a two-step procedure involving two lasers. First, the surgeon creates a small flap in the cornea to prepare the eye for the next step, the vision correction.
The traditional LASIK method of laser vision correction requires a mechanical blade to make the flap.
However, in FEMTOLASIK method we create the flap using the FEMTO LDV™ femtosecond laser. It makes the whole procedure completely blade-free and enables the surgeon to tailor the procedure according to the very unique characteristics of every patient.
Transepithelial Photorefractive Keratectomy
Transepithelial photorefractive keratectomy (or TransPRK for short), represents a very recent iteration of laser refractive surgery. The evolution of this form of surgery started with PRK, which was soon overtaken by LASIK, or laser in situ keratomileusis. The reasons were that LASIK offered much faster recovery of vision and eye comfort than PRK, where recovery was delayed by the need for the surface cells of the cornea to heal. There is also less risk of corneal scarring and refractive regression with LASIK compared with PRK.
There remains a role for PRK, however, as LASIK involves the creation of a corneal flap. This weakens the cornea more than with PRK, where no flap is made. In patients with thinner corneas or where the underlying weakness is suspected, PRK may be a safer option than LASIK.
Originally, during PRK the surface cells of the cornea were scraped off mechanically by a rotating brush, much like an electric toothbrush. Later, these cells were removed in a less traumatic manner by using alcohol to first loosen them, followed by gentle peeling off of the epithelial cells. This form of the surgery is still commonly performed in cases where PRK is chosen as the method of surgery. In order to avoid these extra steps required to remove the surface epithelial cells, a number of doctors and laser companies have attempted to use the excimer laser used to perform refractive surgery to also remove the cells. So far most of these lasers require multiple programming steps by the doctor and also require the doctor to use very subjective signs to tell when the epithelium is removed.
The Schwind Amaris 750S laser can now provide a one step, no touch, TransPRK surgery. Using the TransPRK mode, this laser first removes the surface epithelial cells with the excimer laser and then proceeds immediately with the same laser to remodel the cornea for the refractive correction. Performing surgery in this manner allows all-laser PRK to be carried out in a very short time with minimal manipulation of the eye and in a very gentle way.
Our TransPRK Research Project
The TransPRK method is one of newest refractive surgical techniques by laser, which, for the first time in Iran, was used by Dr. Adib Moghadam employing the SCHWIND Laser Machine. Dr. Adib Moghadam, based on the latest evidence and scientific recommendation in this field, beside employment of years of research and experience, for each individual patient considers the demographic features (like age, sex) and optical characteristics (such as refractive conditions, intensity of refractive conditions, thickness of cornea, aberration, cornea surface, …) and individualize the surgical coordination. In other words, for planning the surgical procedure, a monograph is designed and used which could ascertain how to adapt the steps of the procedure to the status of the patient. This leads to a better result of the surgery qualitatively and quantitatively.
One of the dominant factors in the monogram is the aberration. Aberration in any optical system (as in the eyes) is defined as any distortion of the system performance from the ideal predicted status of the system by the physical-geometrical models. In eye optical system, this phenomenon can lead to disorders like hyperopia, shortsightedness, primary astigmatism, or more profound disorders such as vision distortion, cornea, halo due to spherical aberration and alike conditions. Nowadays, the necessary technology for the assessment of patient’s aberration profile is available. The significance of this matter is due to the fact that assessment of this profile in each patient and considering it in procedure planning step lead to correction not only in the case of low degree aberration but also in the cases of high order aberration. This fact is dominant in the quality of vision correction in each patient.
On the other hand, employment of laser surgery in the case of patients with hyperopia with astigmatism has been always controversial, since the success rate of the surgery and stability of vision status obtained in these patients have not been as good as other patients.
Hyperopia patients: reviewing the follow-up data (1 year after surgery) from the cases of hyperopia that had undergone laser surgery by Dr. Adib Moghadam, revealed that 83% of patients had 90% or better vision; more than 90% of the patients had the eyesight of ±0.5. The finding suggests the effectiveness of this technique and stability of the correction on this group of patients.
Patients with Astigmatism above 0.5: the performed analysis of the cases of patients with astigmatism (above 0.5) who undergone laser surgery by Dr. Adib Moghadam, after their follow-up (two years after surgery) suggests that 85% of the patients had 90% vision or better; 88% of the patients had eyesight of 0.5; 86% of the patients had astigmatism of 0.5 or less. The data claims that the surgical method is effective and provides a stable vision correction in this group of the patients.
By choosing TransPRK, usually, epithelium requires less than 48 hours to repair. The patients gain a vision better than the standard vision, and it is also followed by more satisfactory from the patients. Analysis performed on the preoperative data and the data from follow-up sessions shows that in 6 months after surgery 95% of the patients had the vision of 20/20 or better. Moreover, in 6-month period after the surgery, the degree of the refractive disorder would be about 0.5 for 99% of the patients. All these results suggest high success rate and efficiency of the method.
Based on the analysis, the mean pain intensity in 48 hours after surgery was marked in range of 0 to 2 on a 10-degree scale. This fact also states that the pain accompany the procedure is minimal. Furthermore, the risk of opacity and dryness of cornea was also low, and the light irritability was also improved in the patients. Modification of cornea surface is not significant in these cases. Beside these, avoiding flap creation in this method, improve the symptoms involved with this procedure.
None of the patients who had had their surgery by Dr. Adib Moghadam claims Glare Flare after their surgeries.
The analysis of the patients‘ follow-up data shows that 2 years after the surgery, at least 90% of the patients had the eyesight of 0.5 and 81% of the patients had the vision of better than 90%. These data distinctively states the stability of vision correction after surgery and no recurrence of the refractive condition.
Research Team
This project has been carried out in hospital research centers with professional researchers involved. The results of this study have been presented at national and international conferences such as ESCRS, ASCRS, WOC, MEACO, and AAO. Currently, there are more studies on-going with longer follow-up time to present the data in prestigious international journals. This study is embedded in an international clinical study of patients with TransPRK surgeries, with contribution from Valladolid University, Spain, and Augenklinik Aschaffenburg, Germany.
The researchers contributed to this study include: Dr. Farshad Nourizadeh, Dr. Mehdi Aslani, Dr. Amir Houshang Omidvari, Dr. Bahram Salmanian, Dr. Fatemeh Adili Moghadam, Dr. Saeed Soleimanjahi from Iran, and Dr. Samuel Arba Mosquera and Dr. Roberta Watter-Finke from Germany.
See Dr. Adib Moghaddam publications and lectures here.