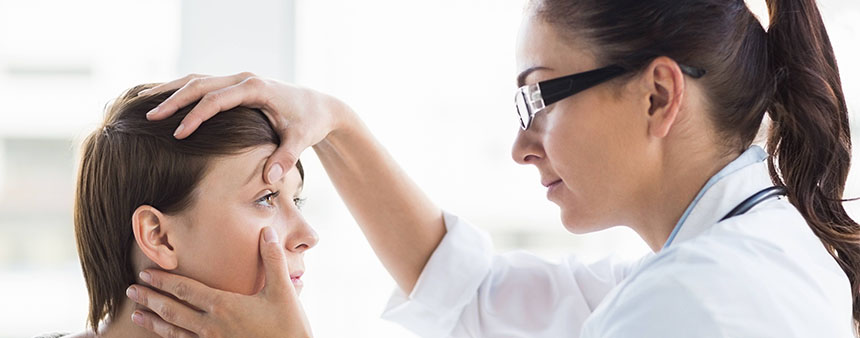
What are the dangers of Keratoconus?
Supervision after refractive errors surgery
2018-08-15
Some of the eye diseases that should not be ignored
2018-09-04Keratoconus is a progressive eye disease in which the normally round cornea thins and begins to bulge into a cone-like shape. This cone shape deflects light as it enters the eye on its way to the light-sensitive retina, causing distorted vision. Doctors do not know for sure why people have Keratoconus. Keratoconus can occur in one or both eyes and often begins during a person’s teens or early 20s. The vision symptoms slowly get worse over a period of about 10 to 20 years.
New research suggests the weakening of the corneal tissue that leads to keratoconus may be due to an imbalance of enzymes within the cornea. This imbalance makes the cornea more susceptible to oxidative damage from compounds called free radicals, causing it to weaken and bulge forward.
Risk factors for oxidative damage and weakening of the cornea include a genetic predisposition, explaining why keratoconus often affects more than one member of the same family. Keratoconus also is associated with overexposure to ultraviolet rays from the sun, excessive eye rubbing, a history of poorly fitted contact lenses and chronic eye irritation.
As the cornea becomes more irregular in shape, it causes progressive nearsightedness and irregular astigmatism to develop, creating additional problems with distorted and blurred vision. Glare and light sensitivity also may occur. Often, keratoconic patients experience changes in their eyeglass prescription every time they visit their eye care practitioner.
Keratoconus can be diagnosed through a routine eye exam. Your ophthalmologist will examine your cornea, and may measure its curve. This helps show if there is a change in its shape. Your ophthalmologist may also map your cornea’s surface using a special computer. This detailed image shows the condition of the cornea’s surface.
There are 5 distinct stages of keratoconus development in the cornea, and each stage needs to be addressed differently. The 5 stages are: Pre-keratoconus; Mild; Moderate; Severe; Corneal transplant surgical.
When your symptoms are mild, your vision can be corrected with eyeglasses. Later you may need to wear special hard contact lenses to help keep vision in proper focus. There are other therapies such as Intacs or Collagen cross-linking that your eye specialist may prescribe with the level of progression of the cornea.
Although Keratoconus usually does not lead to complete blindness, it can reduce the level of vision so that the normal life of the individual is difficult. So, if you have at least one of the symptoms of Keratoconus, it is best to go to a specialist doctor and get an examination.
Reference:
Don’t Risk Serious Vision Problems with Inadequate Keratoconus Treatment
https://www.aao.org/eye-health/diseases/keratoconus-cause
https://www.allaboutvision.com/conditions/keratoconus.htm
https://www.umkelloggeye.org/conditions-treatments/keratoconus